Physician-first
Augmenting clinical teams and handling routine tasks, not replacing human care.
Lumeris is a physician-first healthcare transformation company based in St. Louis, Missouri, with more than 15 years of proven leadership in healthcare operations and value-based care enablement.
Founded by doctors and guided by deep clinical, operational, and technical expertise, we help health systems and physician organizations deliver better outcomes, lower costs, and a better experience for patients and providers.
Today, we’re combining our legacy of success with the power of AI to pioneer Primary Care as a Service (PCaaS)—expanding access, reducing burden, and making it easier for physicians to focus on what matters most: caring for people.
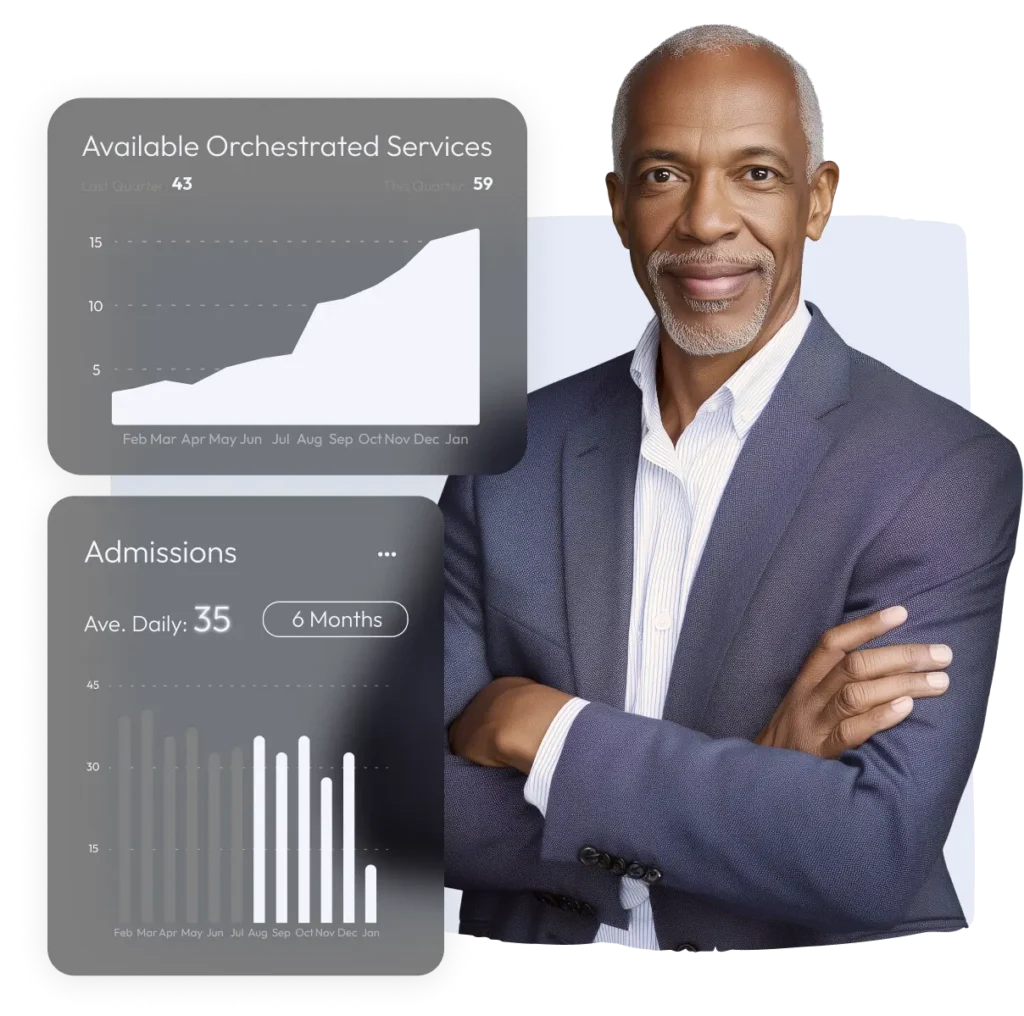
Empowering primary care delivery for health systems
Now, Tom’s reach goes beyond value-based care models. It’s designed to work for every health system, every physician, and every patient — whether in Medicare Advantage, ACO REACH, commercial, or fee-for-service settings. It’s primary care that is:
Enabling physician well-being to unlock better care
For more than 15 years, we’ve partnered with health systems and physician organizations to support the people at the center of care: doctors. Our technology and services reduce burden, improve satisfaction, and restore clinical time—so physicians can focus on what matters most. When doctors are healthy, supported, and practicing at the top of their license, patients receive better care. It’s how we create healthier people from the inside out.


Improving access and experience through responsible AI
We use AI to bridge the gap between visits—so doctors stay better connected to patients, and patients get more from their doctor and care team. Every patient deserves easier access to primary care, stronger continuity, and a better overall experience. Technology should bring care closer—not get in the way. Our platform acts as a bridge, not a barrier—keeping patients engaged between appointments, surfacing the right insights at the right time, and making in-person time more meaningful. The result: fewer gaps, more trust, and coordinated care that patients remember—and return to.
We see a future where Agentic AI delivers digital labor that handles the details, so humans can handle the healing. Where physicians have the time and insight to connect, guide, and inspire change. And where the business of healthcare supports — not hinders — the human touch and the art of medicine.